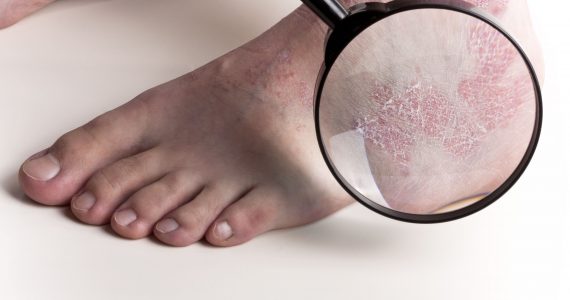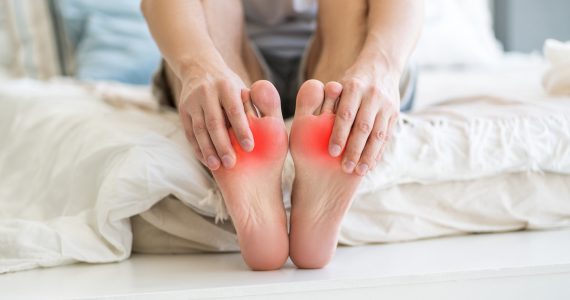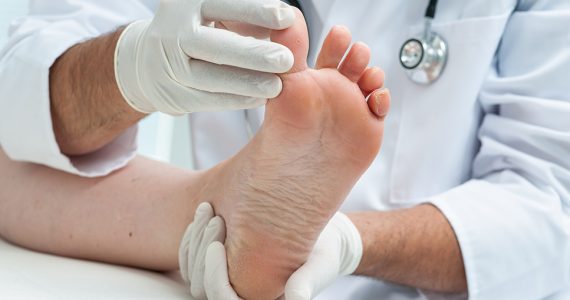
What is athlete’s foot?
Athlete’s foot (Tinea Pedis or ringworm of the foot) is a contagious mycotic infection caused by a dermatophyte fungus: Tinea Pedis.
This type of foot fungus is very common among athletes and sportspeople that frequent hot, humid and public places.
Transmission of the fungus in question takes place:
- Directly: by coming into contact with fragments of skin that are shed by individuals with the fungal infection.
- Indirectly: by coming into contact with showers, footboards, floors or other objects used by persons suffering from the fungal infection.
Athlete’s foot is a very common pathology and mostly affects the male adult and elderly population.
What are the symptoms of athlete’s foot?
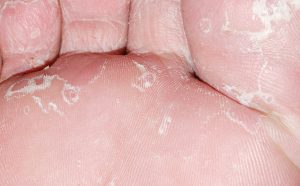 Athlete’s foot can show itself through various types of symptoms; in the early stages the fungal infection usually takes up residence in the infradigital area (between the toes) and may subsequently spread to the sole, top of the foot and the nails with the risk of becoming chronic.
Athlete’s foot can show itself through various types of symptoms; in the early stages the fungal infection usually takes up residence in the infradigital area (between the toes) and may subsequently spread to the sole, top of the foot and the nails with the risk of becoming chronic.
Heat and humidity are factors that encourage the spread of microorganisms that take up residence in the most superficial layers of the skin where the fungus originates.
The fungal infection has typical traits, among the most common are:
- Peeling skin, especially between the toes and on the sole of the foot
- Malodorous feet
- Erythema
- Skin redness
- Itching
- Thickening and weakening of the nails
- Skin thickening
If left untreated, this pathology can create skin lesions with the consequent formation of bacterial infections. The microorganisms responsible for the fungal infection feed on the substance that cover and protect the skin, nails and hair: keratin, paving the way into the epidermal layer for other types of bacteria that that can take up residence in deeper areas until an infection is created.
What are the causes of athlete’s foot?
The fungal infection responsible for athlete’s foot can be caused by endogenous factors (within the body) and exogenous factors (originating outside the body, to do with environmental conditions).
The most common endogenous factors are:
- Weak or debilitated Immune defences
- Existing pathologies such as: AIDS, diabetes, circulatory problems and dermatitis
- Genetic factors (in all probability the individual will have a genetic predisposition to the infection)
The most usual exogenous factors are:
- A build-up of humidity (wet socks or shoes)
- The summer season and hot-humid environments
- Inappropriate footwear and socks (too tight or that do not allow the feet to breathe)
- Walking barefoot in public places
- Hygiene
Treatment and Prevention of Athlete’s foot
Tinea pedis is not an infection that will heal on its own and so treatment it is absolutely necessary. Cures may consist of medication involving the use of antifungal substances, either applied topically or taken orally, or preventive treatment aimed at eradicating the factors that facilitate microbial contamination of the sole of the foot, i.e. maceration of the skin of the feet enclosed in shoes.
There are various substances that exert an antifungal action:
- Among the most common medications are: Sulconazole or Clotrimazole, in the form of ointments, creams or sprays to be applied directly to the infected areas.
- There may be cases in which topical treatment on its own is not enough. In such cases antifungal medications can be taken by mouth which, although their action is shorter, may also have side effects worth taking note of (allergic reactions, gastrointestinal problems, migraines, etc.).
- There are also various substances that act as natural antifungals; preparations containing undecylenic acid, phytosphingosine, usnic acid and triclosan – bronopol are very effective as these act as bio-inhibitors of microbial growth and therefore limit the risk of onychomycosis.
To prevent the onset of Tinea Pedis certain rules of conduct should be followed:
- be careful not to walk around barefoot in very populated spaces;
- keep the feet clean and dry;
- use clean and personal towels;
- wear well-ventilated shoes;
- change socks often.