The nail
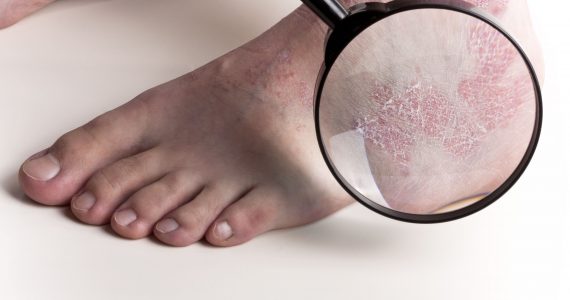
The nail is the thin and slightly convex four-sided plate located on the ends of our fingers and toes. Comprised mainly of keratin (and lower percentages of fats, amino acids, water, vitamins and minerals), its reddish colour is due to the colour of the blood that transpires from the skin, but if it detaches from the nail bed it takes on the yellowish colour typical of horny substances.
It starts from the periosteum and is anchored to the nail bed by its three margins, the most important of which is the top one where the matrix is located that is responsible for nail growth (which is weekly for the fingernails and monthly for toenails). The light pink half-moon at the base of the nail plate is called the lunula.
The nail consists of a front visible part that incorporates: the nail body, the lunula and the cuticle (the fold of skin that encloses the deep regions); the back of the nail is not visible and is made up of the matrix formed by the deep skin surrounding the base of the nail and on which almost all the visible part rests.
The nails perform a series of important functions for our body including:
- protection from trauma;
- maintaining the tactile sensitivity of the fingertip;
- assisting actions involving use of the fingers.
What is onychomycosis?
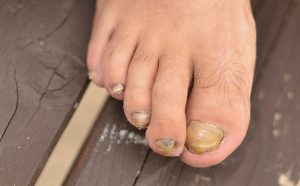 Onychomycosis (mycosis of the nails, otherwise known as Tinea unguium) or more commonly called nail fungus, is an infection that affects the nails (nail plate), of both the hands and feet, and may be caused by a variety of pathogenic agents (dermatophytes, yeasts and moulds).
Onychomycosis (mycosis of the nails, otherwise known as Tinea unguium) or more commonly called nail fungus, is an infection that affects the nails (nail plate), of both the hands and feet, and may be caused by a variety of pathogenic agents (dermatophytes, yeasts and moulds).
The symptoms of this infection are thickening, deformity and a certain discolouration of the nails.
Nail mycoses account for around 50% of all pathologies relating to the nails and the main risk factors are:
- old age
- intimacy
- bad health in general (e.g. diabetics)
- heredity
- frequent use of public showers or swimming pools
- trauma in the area of the nails
- a hot and humid climate
- various types of immune system problem
- athlete’s foot
- psoriasis
The statistics show that the majority of the population affected by nail mycoses (nail fungi) are male and that at least 70% of athletes (sport: basketball) suffer from this pathology.
Athletes are especially more at risk as their nails are continually subjected to microtrauma and often kept in environments that encourage the spread of parasites (hot and sweaty shoes, shared changing rooms, swing pool water, etc.).
Onychomycosis is quite contagious and rarely heals spontaneously. Depending on how severe it is, it may have an important impact on the quality of life of the individuals affected by it.
Considering the nature of the illness and the effect it can have on the individual’s appearance, it can have quite an impact on interpersonal relations. In the most severe cases, the individual may even develop forms of anxiety.
What are the causes of onychomycosis?
The pathogenic agents responsible for around 90% of all nail fungi are dermatophytes, primarily Trichophyton rubrum and Trichophyton mentagrophytes; more rarely the pathology can be attributed to yeasts, non-dermatophyte moulds and Candida.
Onychomycoses caused by yeasts above all affect individuals who keep their hands in water for long periods (bar workers, housewives, fishermen, etc.); while those caused by opportunist moulds (for example, Scopulariopsis brevicaulis and Aspergillus spp.) affect the elderly and clinically simulate onychomycoses from dermatophytes
Prevention and Treatment of onychomycosis
Prevention
Prevention can help us to limit the onset of nail fungi and can be summed up in 3 basic points:
- Correct hygiene and drying prevent the spread of pathogenic agents that cause the mycoses.
- Footwear and socks that ensure good transpiration and ventilation. Socks must be changed frequently to make sure the feet do not remain damp for long periods.
- For individuals who are at risk it is advisable avoid contact with surfaces of public showers and swimming pools and baths.
Treatment
The choice of type of treatment basically depends on the form of the pathology, the severity of the clinical diagnosis and the number of nails impacted by the infection.
Depending on the type of onychomycosis, topical therapy may need to be backed up by oral medication. Systemic therapy, where necessary, consists of taking specific medications (antimycotics) that will inhibit the growth of fungus-like organisms, such as yeasts and moulds. Topical therapy is essential to initially contain and then weaken the infective cause of onychomycosis.